Healthcare expenses can devastate family finances, often forcing difficult choices between medical treatment and daily necessities. The CM Punjab Sehat Sahulat Program eliminates this dilemma by offering free, cashless healthcare up to Rs. 1 million per family to all permanent residents of Punjab. This comprehensive guide walks you through every aspect of the program, from checking your eligibility via SMS to understanding coverage for specific conditions like diabetes and kidney disease, ensuring you can access the life-saving benefits you deserve.
Key Takeaways
- CNIC is Your Sehat Card: No physical card is needed. Your original Computerized National Identity Card serves as the entry point for all program benefits at empaneled hospitals.
- Coverage up to Rs. 1 Million: Each family receives annual coverage starting at Rs. 60,000 for secondary care and extending to Rs. 400,000 for priority treatments, with top-ups for life-threatening conditions reaching Rs. 1 million.
- Free Insulin and Dialysis Available: Diabetic patients receive free insulin during admissions, while kidney patients access free dialysis sessions through the CM Dialysis Program, part of this broader initiative.
- Check Eligibility via 8500 SMS: Send your CNIC number to 8500 and receive an instant reply confirming your eligibility status and available balance.
- Private Hospitals Are Primary Providers: Following recent policy updates, treatment is now primarily available at empaneled private hospitals, while public hospitals continue providing free care through separate government funding.
- Program Continues Despite Rumors: The Sehat Card has not been discontinued. Policy changes only affect service delivery points, not the program’s existence or your entitled benefits.
- Read More: CM Punjab Dialysis Card | Free Dialysis Scheme (by CM Punjab)
- Read More: Maryam Nawaz Insulin Program | Free Insulin Scheme (By Insulin Card)
- Read More: CM Punjab Climate Internship Program (PKR 60K Apply Online)
CM Punjab Sehat Sahulat Program | Free Medicines & Treatments
Table Of Contents
What exactly is the CM Punjab Sehat Sahulat Program and how does it work?

The CM Punjab Sehat Sahulat Program is a government-funded health insurance initiative providing completely free, cashless inpatient treatment to all permanent residents of Punjab province. Managed by the Punjab Health Initiative Management Company, this program eliminates out-of-pocket expenses for hospitalization, surgeries, and major treatments at empaneled private hospitals across Pakistan.
The program operates on a simple principle: your Computerized National Identity Card functions as your health card. When you visit an empaneled hospital with your original CNIC, the hospital facilitation officer verifies your eligibility through a centralized database. Once confirmed, the hospital provides all necessary treatment, medicines, and diagnostics without charging you anything. The government directly reimburses the hospital for all covered expenses.
Key operational features include:
- Cashless Transactions: Patients pay nothing at the point of care. The entire billing process occurs between the hospital and program administrators.
- Family-Based Coverage: The program covers the entire family unit, including husband, wife, and unmarried children, with no limits on family size.
- Pre-Existing Condition Coverage: All medical conditions, regardless of when they developed, receive full coverage under the program.
- Inter-District Portability: Beneficiaries can access treatment at any empaneled hospital across Punjab, not just in their home district.
The program represents Pakistan’s largest healthcare reform effort, targeting universal health coverage for Punjab’s population of over 110 million people. By removing financial barriers to hospitalization, it ensures that life-saving treatments reach those who need them most, regardless of their economic status.
Is the Sehat Card free for all residents of Punjab?

Yes, the Sehat Card is completely free for all permanent residents of Punjab. The government covers the entire premium cost from provincial revenues, requiring no contributions from beneficiaries. This universal coverage model represents a significant departure from traditional insurance programs that charge premiums or require co-payments.
Eligibility extends to every individual holding a valid NADRA-issued CNIC with a permanent Punjab address. This includes:
- Urban and Rural Residents: Coverage applies equally to city dwellers and rural populations across all 36 districts.
- All Income Levels: Unlike earlier versions that targeted only low-income families, the current program has no income restrictions.
- Government Employees: Public sector workers and their families receive full coverage alongside private citizens.
- Pensioners and Retirees: Senior citizens maintain eligibility through their existing CNIC records.
The program’s universality ensures that healthcare access depends solely on medical need, not financial capacity. This approach aligns with the Sustainable Development Goal of achieving universal health coverage by 2030.
Has the Sehat Card program been stopped or changed in Punjab?

No, the Sehat Card program has not been stopped. This misconception stems from significant policy changes implemented in mid-2025 that altered how services are delivered, not the program’s existence. The Punjab government continues funding the program fully, with benefits remaining intact for all eligible residents.
The key changes include:
- Suspension in Government Hospitals: From July 1, 2025, the Sehat Card stopped covering treatments in public hospitals to eliminate duplicate government spending. Public hospitals continue providing free care through separate budgetary allocations.
- Focus on Private Hospitals: The program now operates exclusively through empaneled private hospitals, which remain fully accessible to all cardholders. This shift ensures efficient resource utilization while maintaining service quality.
- Inter-Provincial Suspension: The program temporarily suspended coverage outside Punjab, meaning cardholders cannot currently access treatment in other provinces. However, treatment within Punjab continues uninterrupted.
Official statements from the Punjab Health Initiative Management Company repeatedly emphasize that “health card facilities are available across the province without interruption.” The department actively combats rumors by urging citizens to verify information through official channels rather than social media.
Managed by PHIMC: The role of the Punjab Health Initiative Management Company
The Punjab Health Initiative Management Company serves as the implementing authority for the Sehat Sahulat Program. Created specifically to design, manage, and monitor this healthcare initiative, PHIMC handles all operational aspects from hospital empanelment to claims processing.
PHIMC responsibilities include:
- Hospital Network Management: Identifying, evaluating, and empaneling private hospitals that meet quality standards for patient care.
- Database Integration: Maintaining real-time synchronization with NADRA records to ensure accurate eligibility verification.
- Claims Processing: Reviewing and approving hospital claims for reimbursement, ensuring timely payments to healthcare providers.
- Grievance Redressal: Operating helplines and complaint mechanisms to address patient issues and hospital disputes.
- Quality Monitoring: Conducting regular audits of empaneled hospitals to maintain treatment standards and prevent fraud.
The company operates under a board of directors comprising government officials, healthcare experts, and insurance professionals. This multi-stakeholder governance structure ensures balanced decision-making that prioritizes patient welfare while maintaining financial sustainability.
Eligibility, Registration, and Checking Your Status

Who is eligible for the CM Punjab Sehat Sahulat Program?
All permanent residents of Punjab holding a valid Computerized National Identity Card are automatically eligible for the Sehat Sahulat Program. The program uses NADRA’s database to determine residency status, making the verification process seamless and objective.
Eligibility criteria focus on three core requirements:
- Permanent Residency: Your CNIC must show a permanent address within Punjab’s 36 districts. Temporary residents or those with addresses in other provinces do not qualify.
- Valid CNIC: The CNIC must be current and unexpired. Expired cards require renewal at NADRA offices before eligibility can be confirmed.
- Family Registration: Your family members must be correctly listed in NADRA’s family tree system to receive coverage as a unit.
The program specifically includes:
| Eligible Category | Coverage Details |
|---|---|
| Husband and Wife | Both spouses covered automatically |
| Unmarried Children | All children regardless of age if unmarried |
| Newborns | Automatically added if born in empaneled hospitals |
| Divorced/Widowed Daughters | Covered if residing with parents |
| Disabled Family Members | Full coverage with no exclusions |
What if I am a permanent resident but marked ineligible?
If your CNIC shows a Punjab address but the 8500 SMS service returns “ineligible,” the issue almost always lies with NADRA records rather than the program itself. The solution requires updating your information at the nearest NADRA office.
Common data problems include:
- Outdated Family Tree: Missing spouse or children records prevent family coverage. Request a complete family tree update.
- Incorrect Address: Old addresses from other provinces need correction to reflect current Punjab residency.
- Expired CNIC: Renew your card before checking eligibility again.
- Missing Family Members: Newborns not delivered in empaneled hospitals or spouses added after marriage require manual record updates.
After updating your NADRA record, allow 7-10 days for the changes to synchronize with the Sehat Sahulat database. You can then recheck eligibility via SMS or the online portal.
How to Check Sehat Card Eligibility and Balance Online and Via SMS

How do I check my eligibility for the Sehat Card via SMS?
The simplest and most accessible method requires just your CNIC and a mobile phone. Follow these steps:
- Open your phone’s messaging app
- Type your 13-digit CNIC number without spaces or dashes
- Send the message to 8500
- Within minutes, you receive a reply confirming your eligibility status and available balance
The response message indicates:
- “Eligible”: You qualify for full program benefits. The message may also show your coverage limit and remaining balance.
- “Ineligible”: Your record shows issues requiring NADRA updates. The message sometimes includes reason codes explaining the problem.
- “Please visit NADRA”: Specific instruction to update family records before benefits can activate.
This SMS service operates 24/7 and remains the most popular verification method, processing millions of queries monthly.
Sehat Sahulat Program check online Punjab: How to use the web portal
For detailed information beyond basic eligibility, the official PHIMC website offers comprehensive online checking. Access the portal by:
- Visiting the PHIMC official website
- Entering your CNIC number in the designated field
- Completing the simple verification prompt
- Viewing your complete eligibility profile
The online portal displays:
- Family Member List: Names of all covered family members with their CNIC numbers
- Coverage Balance: Current remaining limit for the annual coverage period
- Treatment History: Previous hospital admissions and claims processed under your card
- Nearby Hospitals: Map-based listing of empaneled hospitals in your area
This detailed view helps families plan treatments and understand their coverage status before visiting hospitals.
How to Check Sehat Card Balance via Mobile App
The State Life Health Plus Mobile App provides another convenient option for balance checking. Available for both Android and iOS devices, the app offers:
- Biometric Login: Fingerprint or facial recognition for secure access
- Real-Time Balance: Instant coverage limit updates
- Claim Tracking: Monitor ongoing treatment authorizations
- Hospital Locator: GPS-based directions to nearest empaneled facilities
- Digital Card: Electronic verification proof if you forget physical CNIC
Download the app from official app stores and register using your CNIC and mobile number for secure access.
Understanding “Balance” vs. “Treatment Approval”
A crucial distinction that confuses many beneficiaries involves the difference between available balance and treatment approval. Your balance shows the monetary limit remaining for the year, but final treatment approval depends on medical necessity and hospital capacity.
Important points to remember:
- Balance Shows Maximum: The displayed amount represents the upper limit, not guaranteed payment for any treatment
- Medical Necessity Required: Doctors must confirm hospitalization is medically required
- Hospital Empanelment: Treatment must occur at program-approved facilities
- Package Rates Apply: Hospitals charge pre-negotiated package rates, which may differ from market prices
- Life-Threatening Exception: Emergency treatments continue even if balance exhausts during care
Always confirm treatment approval with the hospital facilitation officer before proceeding, regardless of your displayed balance.
Family Coverage Details
Who is included in a family under the Sehat Sahulat Program?
The program defines “family” broadly to ensure maximum coverage for dependents. Understanding this definition helps verify that all eligible members receive benefits.
The standard family unit includes:
- Head of Household: Usually the husband or eldest earning member
- Spouse: Legally married wife (or husband, if female is head)
- Unmarried Children: Sons and daughters regardless of age, as long as they remain unmarried
- Divorced/Widowed Daughters: Covered if residing with and dependent on parents
- Orphaned Grandchildren: May qualify if living with and dependent on grandparents
- Disabled Family Members: Full coverage regardless of age or marital status with proper medical documentation
The program imposes no upper limit on family size. Large families with multiple children receive the same coverage amount as smaller families, with the annual limit applying collectively rather than per individual.
How can I add a missing family member to the Sehat Card records?
Adding missing family members requires updating NADRA records first, followed by synchronization with the program database. The process varies depending on the member type:
For newborns delivered in empaneled hospitals:
- The hospital automatically registers the birth with NADRA
- The newborn appears in your family record within days
- No additional action required from parents
For newborns delivered elsewhere:
- Obtain Form-B from the union council where birth occurred
- Visit NADRA with Form-B and parents’ CNICs
- Request child’s registration in your family tree
- Allow 7-10 days for program database update
For new spouses after marriage:
- Register marriage with NADRA by submitting marriage certificate
- Request spouse addition to your family tree
- Verify updated record after 2-3 weeks
For elderly parents:
- Ensure parents are listed in your family tree at NADRA
- If not, visit NADRA with their CNICs and relationship proof
- Request family tree modification
Remember that only NADRA additions trigger program updates. The Sehat Sahulat database automatically synchronizes with NADRA, eliminating any need for separate registration with PHIMC.
Read More: Honhaar Jawan Program (Free IT Courses, Laptops, & Solar Panels)
CM Punjab Transplant Program Hospital List
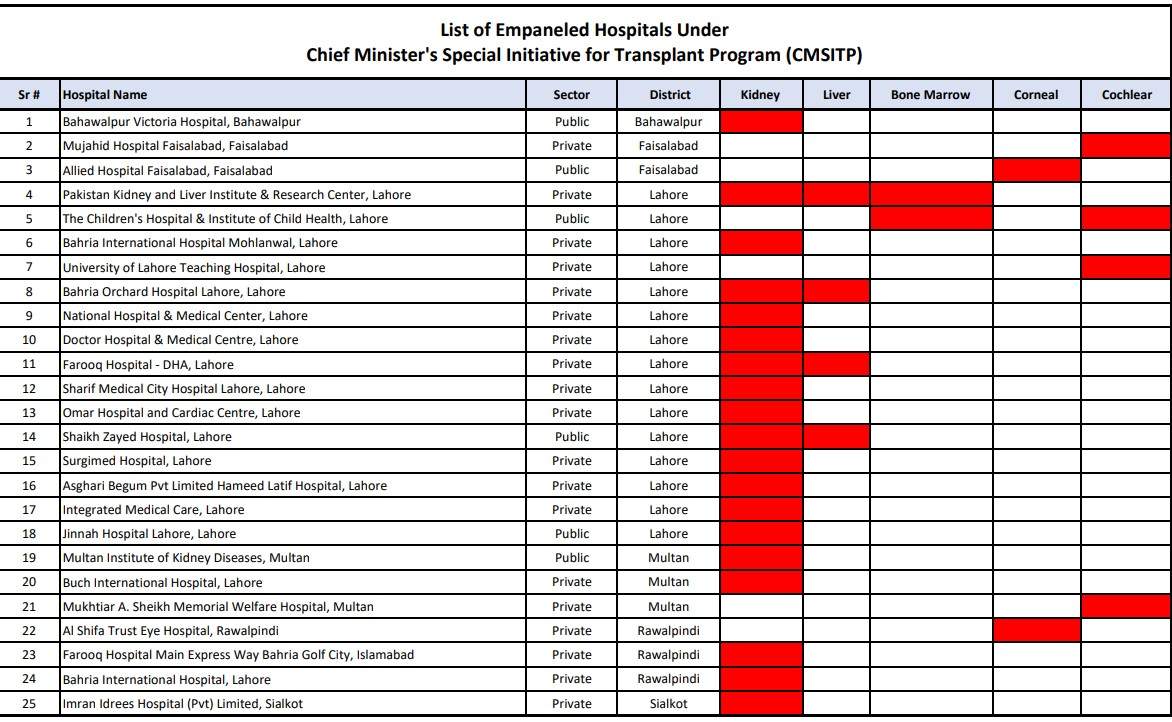
| Hospital Name | Sector | District | Kidney | Liver | Bone Marrow | Corneal | Cochlear |
|---|---|---|---|---|---|---|---|
| Bahawalpur Victoria Hospital | Public | Bahawalpur | Yes | No | No | No | No |
| Mujahid Hospital Faisalabad | Private | Faisalabad | No | No | No | Yes | Yes |
| Allied Hospital Faisalabad | Public | Faisalabad | No | No | Yes | No | No |
| Pakistan Kidney and Liver Institute & Research Center | Private | Lahore | Yes | Yes | Yes | No | No |
| The Children’s Hospital & Institute of Child Health | Public | Lahore | No | No | Yes | Yes | Yes |
| Bahria International Hospital Mohlanwal | Private | Lahore | Yes | No | No | No | No |
| University of Lahore Teaching Hospital | Private | Lahore | No | No | No | Yes | Yes |
| Bahria Orchard Hospital Lahore | Private | Lahore | Yes | Yes | No | No | No |
| National Hospital & Medical Center | Private | Lahore | Yes | No | No | No | No |
| Doctor Hospital & Medical Centre | Private | Lahore | Yes | No | No | No | No |
| Farooq Hospital – DHA | Private | Lahore | Yes | Yes | No | No | No |
| Sharif Medical City Hospital Lahore | Private | Lahore | Yes | No | No | No | No |
| Omar Hospital and Cardiac Centre | Private | Lahore | Yes | No | No | No | No |
| Shaikh Zayed Hospital | Public | Lahore | Yes | Yes | No | No | No |
| Surgimed Hospital | Private | Lahore | Yes | No | No | No | No |
| Asghari Begum Pvt Limited Hameed Latif Hospital | Private | Lahore | Yes | No | No | No | No |
| Integrated Medical Care | Private | Lahore | Yes | No | No | No | No |
| Jinnah Hospital Lahore | Public | Lahore | Yes | No | No | No | No |
| Multan Institute of Kidney Diseases | Public | Multan | Yes | No | No | No | No |
| Buch International Hospital | Private | Multan | Yes | No | No | No | Yes |
| Mukhtiar A. Sheikh Memorial Welfare Hospital | Private | Multan | No | No | No | Yes | Yes |
| Al Shifa Trust Eye Hospital | Private | Rawalpindi | No | No | No | Yes | No |
| Farooq Hospital Main Express Way Bahria Golf City | Private | Rawalpindi | Yes | No | No | No | No |
| Bahria International Hospital | Private | Rawalpindi | Yes | No | No | No | No |
| Imran Idrees Hospital (Pvt) Limited | Private | Sialkot | Yes | No | No | No | No |
Public / Government Hospitals Empaneled Under CM Punjab Transplant Program

| Hospital Name | District | Kidney | Liver | Bone Marrow | Corneal | Cochlear |
|---|---|---|---|---|---|---|
| Bahawalpur Victoria Hospital, Bahawalpur | Bahawalpur | Yes | No | No | No | No |
| Allied Hospital Faisalabad | Faisalabad | No | No | Yes | No | No |
| The Children’s Hospital & Institute of Child Health, Lahore | Lahore | No | No | Yes | Yes | Yes |
| Shaikh Zayed Hospital, Lahore | Lahore | Yes | Yes | No | No | No |
| Jinnah Hospital Lahore | Lahore | Yes | No | No | No | No |
| Multan Institute of Kidney Diseases | Multan | Yes | No | No | No | No |
Total Public Hospitals: 6 Key Observation: Public hospitals tend to focus more on kidney, bone marrow, corneal, and cochlear procedures, with strong pediatric and specialized institute presence (e.g., Children’s Hospital Lahore and Shaikh Zayed).
Private Hospitals Empaneled Under CM Punjab Transplant Program

| Hospital Name | District | Kidney | Liver | Bone Marrow | Corneal | Cochlear |
|---|---|---|---|---|---|---|
| Mujahid Hospital Faisalabad | Faisalabad | No | No | No | Yes | Yes |
| Pakistan Kidney and Liver Institute & Research Center, Lahore | Lahore | Yes | Yes | Yes | No | No |
| Bahria International Hospital Mohlanwal, Lahore | Lahore | Yes | No | No | No | No |
| University of Lahore Teaching Hospital, Lahore | Lahore | No | No | No | Yes | Yes |
| Bahria Orchard Hospital Lahore | Lahore | Yes | Yes | No | No | No |
| National Hospital & Medical Center, Lahore | Lahore | Yes | No | No | No | No |
| Doctor Hospital & Medical Centre, Lahore | Lahore | Yes | No | No | No | No |
| Farooq Hospital – DHA, Lahore | Lahore | Yes | Yes | No | No | No |
| Sharif Medical City Hospital Lahore | Lahore | Yes | No | No | No | No |
| Omar Hospital and Cardiac Centre, Lahore | Lahore | Yes | No | No | No | No |
| Surgimed Hospital, Lahore | Lahore | Yes | No | No | No | No |
| Asghari Begum Pvt Limited Hameed Latif Hospital | Lahore | Yes | No | No | No | No |
| Integrated Medical Care, Lahore | Lahore | Yes | No | No | No | No |
| Buch International Hospital | Multan | Yes | No | No | No | Yes |
| Mukhtiar A. Sheikh Memorial Welfare Hospital | Multan | No | No | No | Yes | Yes |
| Al Shifa Trust Eye Hospital | Rawalpindi | No | No | No | Yes | No |
| Farooq Hospital Main Express Way Bahria Golf City | Rawalpindi | Yes | No | No | No | No |
| Bahria International Hospital | Rawalpindi | Yes | No | No | No | No |
| Imran Idrees Hospital (Pvt) Limited | Sialkot | Yes | No | No | No | No |
Total Private Hospitals: 19 Key Observation: Private hospitals dominate the list (especially in Lahore), providing the majority of kidney, liver, corneal, and cochlear services. This public-private partnership significantly expands capacity and geographic reach under the free transplant scheme.
Complete Guide to Treatment Coverage and Exclusions
What medical treatments and services are covered under the Sehat Card?
The Sehat Sahulat Program covers an extensive range of inpatient medical services, focusing on conditions requiring hospitalization. Coverage emphasizes life-saving and life-altering treatments that would otherwise impose catastrophic financial burdens on families.
Covered services include:
- Emergency Room Visits: When emergencies lead to hospital admission, all ER costs are covered
- Surgeries: Both elective and emergency surgical procedures
- Intensive Care: ICU, CCU, and NICU stays with all associated costs
- Cancer Treatment: Chemotherapy, radiotherapy, and cancer-related surgeries
- Cardiac Care: Angioplasty, bypass surgery, and heart valve replacements
- Dialysis: Regular dialysis sessions for kidney failure patients
- Thalassemia Treatment: Blood transfusions and iron chelation therapy
- Accident Care: Trauma surgery, fracture management, and prosthesis
- Infectious Diseases: Treatment for Hepatitis, HIV, and severe infections
- Diabetes Complications: Management of diabetic emergencies and complications
How much coverage is provided per family annually?
The program offers tiered coverage limits designed to address varying medical needs while ensuring financial sustainability:
| Coverage Tier | Annual Limit | Applicable Conditions |
|---|---|---|
| Secondary Care | Rs. 60,000 | General medical admissions, minor surgeries |
| Priority Care | Rs. 400,000 | Major surgeries, cardiac procedures, cancer care |
| Life-Threatening Extension | Up to Rs. 1,000,000 | Critical conditions requiring extended treatment |
| Special Case Approval | Beyond Rs. 1,000,000 | Exceptional circumstances reviewed case-by-case |
The limits renew automatically each year on the anniversary of your first treatment or on a fixed date determined by program administrators. Unused coverage does not accumulate or convert to cash.
What happens if my treatment cost exceeds the coverage limit?
The program includes safeguard provisions for patients whose treatment costs exceed standard limits. These protections ensure that patients do not face abandonment mid-treatment due to exhausted coverage.
Protection mechanisms include:
- Ongoing Treatment Continuation: If your limit exhausts during an admission, your current treatment continues until medical discharge
- Life-Threatening Extension: Critical conditions automatically qualify for extended coverage up to Rs. 1,000,000
- Special Appeal Process: Hospitals can request additional coverage for exceptional cases through PHIMC review
- No Patient Abandonment: Empaneled hospitals contractually cannot discharge patients solely due to limit exhaustion
These protections apply specifically to life-threatening conditions and ongoing treatments. Elective procedures scheduled after limit exhaustion require either coverage renewal or alternative payment arrangements.
Specialized Disease Coverage
How can kidney patients get free dialysis through the CM Punjab program?
Kidney patients receive comprehensive dialysis coverage through the CM Dialysis Program, a specialized initiative operating under the Sehat Sahulat umbrella. This program targets the over 800,000 Punjab residents suffering from chronic kidney disease who require regular dialysis sessions.
Dialysis coverage includes:
- Hemodialysis Sessions: Regular in-center dialysis at empaneled hospitals
- Peritoneal Dialysis Supplies: Equipment and solutions for home-based dialysis
- Medications: Essential drugs administered during dialysis
- Lab Tests: Routine blood work to monitor treatment effectiveness
- Vascular Access: Surgical procedures for fistula creation and maintenance
- Emergency Dialysis: Unscheduled sessions for acute kidney injury
The program recently increased annual funding for dialysis patients from Rs. 700,000 to Rs. 1,000,000, ensuring uninterrupted treatment for even the most complex cases. Patients receive dialysis at over 150 empaneled centers across Punjab, with new centers added regularly in underserved districts.
Does the Sehat Card cover free insulin for diabetic patients?
Yes, diabetic patients receive free insulin and diabetes management supplies when admitted to hospitals for diabetes-related complications. The coverage extends beyond simple insulin provision to comprehensive diabetes care during hospitalization.
Covered diabetes services include:
- Insulin Administration: All insulin types prescribed during admission
- Blood Glucose Monitoring: Test strips and monitoring equipment
- Diabetes Education: In-hospital counseling on diabetes management
- Complication Treatment: Care for diabetic foot ulcers, ketoacidosis, and hypoglycemia
- Specialist Consultations: Endocrinologist and diabetes specialist fees
- Follow-Up Care: Post-discharge medications for up to five days
For outpatient insulin needs, the government recently announced a new initiative delivering insulin to Type 1 diabetic patients at their doorsteps. This program complements the Sehat Card’s inpatient coverage, ensuring comprehensive diabetes care across all settings.
Is heart surgery covered under the Sehat Sahulat Program?
Heart surgeries receive full coverage under the program, including both routine and complex cardiac procedures. Thousands of patients have already benefited from free cardiac care, with many receiving life-saving surgeries they could never afford independently.
Covered cardiac procedures include:
- Angioplasty and Stenting: Balloon dilation and stent placement for blocked arteries
- Coronary Artery Bypass Grafting: Open-heart surgery to bypass blocked vessels
- Valve Replacement: Surgical or transcatheter valve repair and replacement
- Pacemaker Implantation: Device insertion for rhythm disorders
- Congenital Defect Repair: Surgery for heart defects present since birth
- Diagnostic Procedures: Angiograms, echocardiograms, and cardiac catheterization
A typical case involves patients like Sulakhan Singh, who received three heart stents completely free under the program. Without this coverage, his family would have faced expenses exceeding their annual income, forcing impossible choices between treatment and other necessities.
Is cancer treatment and chemotherapy covered by the Punjab Sehat Card?
Comprehensive cancer care ranks among the program’s highest priorities, covering the full spectrum of oncology services from diagnosis through treatment and follow-up. This coverage has transformed cancer care access for millions of Punjab families.
Cancer coverage includes:
- Chemotherapy: All standard chemotherapy regimens and protocols
- Radiotherapy: External beam radiation and brachytherapy
- Surgical Oncology: Cancer removal surgeries and reconstructive procedures
- Diagnostic Imaging: CT scans, MRIs, and PET scans for staging and monitoring
- Pathology Services: Biopsy analysis and tumor marker testing
- Pain Management: Palliative care and pain control medications
- Targeted Therapy: Selected targeted drugs and immunotherapy agents
The program covers both adult and pediatric cancers, with specialized pediatric oncology units at major hospitals receiving additional support. Over 16,000 cancer treatments were delivered in a single month, demonstrating the program’s massive scale and impact.
Can I get a free kidney transplant through the CM Punjab program?
Kidney transplantation receives coverage as part of the program’s comprehensive kidney disease management. While transplant procedures are covered, they require additional documentation and approval due to their complexity and cost.
Transplant coverage includes:
- Pre-Transplant Evaluation: Comprehensive donor and recipient testing
- Transplant Surgery: The surgical procedure itself with all associated hospital costs
- Immunosuppressive Medications: Post-transplant drugs to prevent rejection
- Follow-Up Care: Regular monitoring for at least one year post-transplant
- Complication Management: Treatment of any post-surgical complications
Patients seeking transplants must undergo evaluation at designated transplant centers empaneled under the program. The transplant team coordinates with program administrators to secure approval before proceeding.
Is eye surgery covered by the Sehat Card?
Essential eye surgeries receive coverage, particularly those addressing conditions that could lead to permanent vision loss. The program focuses on medically necessary procedures rather than cosmetic or refractive surgeries.
Covered eye procedures include:
- Cataract Surgery: Phacoemulsification with intraocular lens implantation
- Glaucoma Surgery: Trabeculectomy and drainage implant procedures
- Retinal Surgery: Repair of retinal detachments and diabetic retinopathy
- Corneal Transplants: Replacement of damaged corneas
- Trauma Repair: Surgical repair of eye injuries
- Pediatric Eye Surgery: Correction of congenital eye conditions
Routine eye exams and prescription eyeglasses are not covered, as these fall under outpatient care excluded from the program.
Does the Sehat Card cover pregnancy and delivery charges?
Maternity coverage under the Sehat Card applies primarily to complicated deliveries requiring hospitalization and surgical intervention. The program distinguishes between routine obstetric care and emergency complications.
Coverage includes:
- Cesarean Sections: Surgical deliveries with all associated hospital costs
- High-Risk Pregnancy Management: Inpatient care for pregnancy complications
- Emergency Obstetric Care: Treatment of hemorrhage, eclampsia, and other emergencies
- Newborn Complications: NICU care for babies requiring intensive support
- Miscarriage Management: Surgical intervention for incomplete miscarriage
Routine vaginal deliveries at public hospitals continue receiving free care through separate government programs. At private empaneled hospitals, normal deliveries may require partial payment depending on specific hospital arrangements.
Exclusions: What is Not Covered

Which treatments are NOT covered by the Punjab Sehat Card?
Understanding exclusions helps patients avoid frustration when seeking care. The program explicitly excludes certain services to focus resources on life-saving inpatient treatments.
The complete exclusion list includes:
- Outpatient Consultations: Routine doctor visits without admission
- Outpatient Medications: Prescriptions filled at pharmacies without hospitalization
- Normal Vaginal Deliveries: Uncomplicated births at private hospitals
- Dental Treatments: Most dental procedures except those related to facial trauma
- Cosmetic Surgery: Purely aesthetic procedures without medical necessity
- Eyeglasses and Contact Lenses: Vision correction devices
- Drug Addiction Treatment: Rehabilitation and detoxification services
- Self-Inflicted Injuries: Injuries resulting from suicide attempts
- Crime-Related Injuries: Injuries sustained during criminal activity
- Experimental Treatments: Unproven therapies not in standard protocols
- Infertility Treatment: IVF and other fertility procedures
Patients requiring excluded services must arrange alternative payment or seek care at public hospitals where many excluded services remain available free through other government programs.
How to Use the Sehat Card at Empaneled Hospitals
Which hospitals in Punjab accept the Sehat Sahulat Card?
Hundreds of empaneled hospitals across all Punjab districts accept the Sehat Card, providing extensive geographic coverage. The hospital network includes both large tertiary care centers and smaller community hospitals, ensuring access even in rural areas.
Hospital types in the network:
- Tertiary Care Hospitals: Major medical centers offering specialized services like cardiac surgery and cancer treatment
- District Headquarters Hospitals: Secondary care facilities in district capitals
- Tehsil-Level Hospitals: Community hospitals serving sub-district populations
- Specialty Hospitals: Facilities focused on specific areas like cardiology, oncology, or ophthalmology
- Private Teaching Hospitals: Medical college-affiliated hospitals with advanced capabilities
Major cities have dozens of empaneled hospitals, while smaller towns typically have at least one participating facility. The complete list, regularly updated on the PHIMC website, includes hospital names, addresses, contact numbers, and available specialties.
How can I find the list of empaneled hospitals in my city?
Finding nearby empaneled hospitals requires just a few minutes using available tools:
- Online Portal: Visit the PHIMC website and navigate to the “Empaneled Hospitals” section. Search by district, tehsil, or hospital name for complete listings.
- Mobile App: The State Life Health Plus App includes a hospital locator showing nearby facilities on a map with directions.
- Helpline: Call 0800-09009 and provide your city name to receive hospital recommendations from trained operators.
- SMS Service: Send your city name to designated numbers for a list of local hospitals.
The online portal offers the most comprehensive information, including:
- Hospital contact details and visiting hours
- Available specialties and services
- Doctor lists and consultation schedules
- Patient reviews and quality ratings
- Directions and transportation options
Can I use the Sehat Card in private hospitals?
Yes, private hospitals form the primary service delivery network for the Sehat Sahulat Program following recent policy updates. These facilities offer several advantages over public hospitals, including shorter wait times, more comfortable accommodations, and often more advanced technology.
Private hospital participation benefits:
- Reduced Public Hospital Burden: Private facilities absorb cases that would otherwise overwhelm government hospitals
- Geographic Distribution: Private hospitals exist in areas lacking public facilities
- Choice and Competition: Patients can choose among multiple providers, encouraging quality improvement
- Specialized Services: Many private hospitals offer niche specialties unavailable in public sector
Treatment at private hospitals follows the same process as public facilities. Present your CNIC at the hospital’s Sehat Sahulat desk, verify eligibility, and receive treatment without any payment. The hospital bills the program directly for all covered services.
Is the Sehat Card valid for residents of other provinces living in Punjab?
The program covers only permanent Punjab residents verified through NADRA records. Individuals with CNICs showing addresses in other provinces do not qualify, even if currently living in Punjab temporarily.
Exceptions apply for:
- Government Employees: Federal employees posted in Punjab may qualify with proper documentation
- Students: Out-of-province students studying in Punjab remain covered by their home province programs
- Temporary Workers: Short-term workers should maintain coverage through their home province schemes
Each Pakistani province operates its own health card program. Residents should verify coverage through their home province’s system rather than expecting Punjab program access.
Can I use the Sehat Card anywhere in Pakistan?
Currently, the Punjab Sehat Card only provides coverage within Punjab province. Inter-provincial portability was suspended in July 2025, meaning cardholders cannot access treatment at empaneled hospitals in other provinces or territories.
The suspension affects:
- Islamabad: Federal capital hospitals no longer accept Punjab Sehat Cards
- Khyber Pakhtunkhwa: Previously accessible hospitals in KP are now unavailable
- Sindh: Karachi and other Sindh hospitals have stopped Punjab card acceptance
- Balochistan: Limited previous access has been suspended
- AJK and GB: Azad Kashmir and Gilgit-Baltistan facilities no longer participate
Patients already receiving treatment before the suspension date were permitted to complete their care. New treatments outside Punjab require either payment or coverage through the destination province’s health card if eligible.
Step-by-Step Treatment Process
How do I get treatment using my Sehat Card?
Follow this complete step-by-step guide to ensure smooth treatment access:
Step 1: Verify Eligibility Before Travel
Send your CNIC to 8500 or check online to confirm active eligibility. Note your remaining balance and any special conditions.
Step 2: Select an Empaneled Hospital
Choose a hospital from the official list that offers services matching your medical needs. Call ahead to confirm they accept Sehat Card patients for your specific condition.
Step 3: Gather Required Documents
Bring these items to the hospital:
- Original CNIC (mandatory, no copies accepted)
- Previous medical records and test results
- Doctor referrals if you have them
- List of current medications
Step 4: Visit Hospital Sehat Desk
Upon arrival, proceed to the designated Sehat Sahulat Facilitation Desk. Identify yourself as a program beneficiary seeking admission.
Step 5: Complete Verification
The Hospital Facilitation Officer will:
- Scan or enter your CNIC in the system
- Verify eligibility and available balance
- Confirm the hospital’s ability to provide required treatment
- Generate a treatment authorization if approved
Step 6: Doctor Consultation
Meet with the attending doctor who will:
- Evaluate your condition
- Determine if admission is medically necessary
- Order initial tests if required
- Document findings for program records
Step 7: Admission Processing
If admission is approved:
- Complete hospital admission forms
- Receive your room assignment
- Begin treatment as ordered
- Understand that no payment is required at any point
Step 8: During Hospital Stay
Throughout your admission:
- All medicines, tests, and procedures are provided free
- The hospital coordinates with program administrators for any extended coverage needs
- You can request assistance from the Hospital Facilitation Officer if issues arise
Step 9: Discharge and Follow-Up
At discharge:
- Receive discharge summary and prescriptions
- Get up to five days of post-discharge medications covered
- Understand any follow-up appointment requirements
- Confirm that no bills or payments are due
Step 10: Post-Discharge Support
After leaving:
- Contact helpline if you experience any issues
- Return for follow-up as scheduled
- Check your updated balance for future needs
What should I know before going to the hospital?
Preparation significantly improves your hospital experience. Keep these points in mind:
- Original CNIC Required: No exceptions. Photocopies, expired cards, or other ID forms will not work.
- Admission Required: The program covers only inpatient care. OPD visits and pharmacy-only trips are not covered.
- Emergency Access: For emergencies, go directly to the nearest empaneled hospital. Verification happens after stabilization.
- Hospital Choice: You may choose any empaneled hospital, but confirm they offer your needed services beforehand.
- Transportation: Arrange your own transport. The program does not cover ambulance services.
- Accompaniment: Bring a family member if possible to assist with communication and decisions.
What services are covered during hospitalization?
Once admitted, comprehensive coverage includes:
- Room Charges: Accommodation in general wards or semi-private rooms
- Doctor Fees: Attending physician, surgeon, anesthetist, and consultant fees
- Nursing Care: All nursing services during your stay
- Medications: All prescribed medicines administered during admission
- Surgical Supplies: Operating room charges, instruments, and consumables
- Diagnostic Tests: Laboratory work, imaging, and pathology services
- Blood Products: Transfusions and blood component therapy
- ICU Care: Intensive care with all associated monitoring and treatment
- Medical Devices: Implants, stents, pacemakers, and prostheses
- Dietary Services: Hospital meals modified for medical needs
The coverage continues until medical discharge, regardless of how long your stay extends.
Are medicines, tests, and diagnostics covered?
Yes, all medicines prescribed during hospitalization and all diagnostic tests ordered during admission receive full coverage. This includes:
- Inpatient Medications: IV fluids, injectable drugs, oral medications administered during stay
- Pre-Admission Testing: Tests ordered within one day before admission are covered
- Intra-Procedure Monitoring: Continuous monitoring during surgeries and procedures
- Post-Discharge Medications: Up to five days of medications supplied at discharge
- Routine Lab Work: Daily or frequent testing required for monitoring
- Specialized Testing: Advanced diagnostics like MRIs, CT scans, and biopsies
The key requirement is that all medicines and tests must be ordered while you are admitted or within the one-day pre-admission window. Outpatient prescriptions filled at external pharmacies are not covered.
Grievances, Complaints, and Common Problems
What should I do if a panel hospital refuses Sehat Card treatment?
Hospital refusals sometimes occur, but most can be resolved through proper channels. Follow this escalation path:
Step 1: Understand the Refusal Reason
Ask the hospital to explain specifically why they are refusing. Common legitimate reasons include:
- Your condition does not require admission (outpatient appropriate)
- Your treatment appears on the exclusion list
- The hospital lacks capability for your needed procedure
- Your coverage limit is exhausted for non-emergency care
Step 2: Contact Hospital Facilitation Officer
Every empaneled hospital has an on-site HFO responsible for program coordination. Request their assistance in resolving the refusal. They can:
- Verify if the refusal reason is valid
- Escalate to hospital administration if refusal is inappropriate
- Contact PHIMC for guidance on complex cases
Step 3: Call the Helpline
If the HFO cannot resolve the issue, call 0800-09009 immediately. Provide:
- Your CNIC number
- Hospital name and location
- Reason given for refusal
- Name of refusing doctor or staff member
Helpline operators will contact hospital administration directly to intervene.
Step 4: Email Formal Complaint
Send details to info@phimc.punjab.gov.pk with:
- Complete incident description
- Hospital name and date
- Contact information for follow-up
- Any reference numbers provided
Step 5: Visit PHIMC Office
For serious unresolved issues, visit the PHIMC head office in Lahore with all documentation.
What is the helpline number for Punjab Sehat Sahulat Program complaints?
Multiple contact channels ensure beneficiaries can always reach assistance:
Primary Helpline: 0800-09009
- Available 24 hours daily, including holidays
- Toll-free from all networks
- Multilingual operators including Urdu, Punjabi, and English
Alternate Phone Numbers:
- 0333-6756390 (Mobile)
- 042-99066000 (Landline)
- 042-99066001 (Landline)
- Hours: Monday–Saturday, 8:00 AM to 11:00 PM
Email Support:
- info@phimc.punjab.gov.pk for general inquiries
- complaints@phimc.punjab.gov.pk for grievance filing
- Response within 24-48 hours
Physical Address:
Punjab Health Initiative Management Company
(Address available on official website)
Lahore, Punjab
Social Media:
Official PHIMC accounts on Facebook and Twitter provide updates and accept messages.
Why is my CNIC not eligible even though I live in Punjab?
Ineligibility despite Punjab residency almost always traces to data issues rather than program exclusion. Common causes:
- NADRA Address Still Shows Other Province: If you recently moved to Punjab, your CNIC address may not yet reflect this change.
- Family Tree Not Updated: Marriage, birth, or death records missing from NADRA database.
- Expired CNIC: Cards expired over six months may drop from active databases.
- Temporary Address: Some mobile SIM registrations or utility bills show Punjab, but NADRA still lists another province.
- Name Discrepancy: Minor spelling differences between CNIC and other records can cause verification failure.
Resolution requires visiting NADRA with:
- Proof of Punjab residence (utility bills, rental agreement)
- Old and new CNICs if applicable
- Marriage certificate for spouse addition
- Children’s B-Forms for family tree updates
After NADRA updates, wait 7-10 days and recheck via 8500 SMS.
How do I renew my expired Sehat Card?
Since your CNIC functions as your Sehat Card, renewal simply means renewing your CNIC at NADRA. The process:
- Visit any NADRA registration center with:
- Old/expired CNIC
- Birth certificate or other identity proof
- Recent photographs (though NADRA usually takes fresh photos)
- Complete the CNIC renewal application
- Pay the standard NADRA renewal fee
- Collect your new CNIC after processing (typically 7-15 days)
Once NADRA issues your renewed CNIC, the Sehat Sahulat database automatically updates within approximately two weeks. You can then use your new card for healthcare access.
During the gap between CNIC renewal and database update, keep your old CNIC and renewal receipt. If emergency treatment arises, present both at the hospital, and the facilitation officer can manually verify your eligibility through alternative systems.
Program Statistics and Impact
How many people benefit from the Sehat Sahulat Program?
The program’s scale demonstrates its significance in Punjab’s healthcare landscape:
| Metric | Number |
|---|---|
| Families Enrolled | Over 44 million |
| Total Hospital Visits | More than 16 million |
| Cancer Treatments | Over 16,000 monthly |
| Heart Procedures | Over 2,400 monthly |
| Dialysis Sessions | Available to 812,575+ patients |
| Daily Health Cards Issued | Approximately 60,000 |
| Budget Allocation | Rs. 500+ crore released to insurance partners |
Beneficiary Satisfaction Rates:
- 98% satisfied with treatment received
- 98% satisfied with hospital services
- 98% satisfied with hospital staff behavior
- 99% satisfied with program staff behavior
- 98% not asked to pay during treatment
These high satisfaction rates reflect the program’s successful implementation and positive impact on millions of lives. Patients consistently report relief at receiving quality care without financial stress.
Frequently Asked Questions
Will I get cash if I don’t use my coverage?
No. The Sehat Sahulat Program provides health insurance, not cash payments. Unused coverage has no cash value and cannot be withdrawn, transferred, or converted to any other form. The benefit exists only as protection against future medical expenses. Think of it like car insurance: you pay premiums to cover potential accidents, not to receive cash if you drive safely.
Is there an age limit to benefit from the Sehat Card?
No age restrictions apply. Newborns receive coverage immediately upon birth registration, while senior citizens in their 90s and beyond continue receiving full benefits. The program covers all ages equally, recognizing that healthcare needs span the entire lifespan. Pediatric care for children and geriatric care for the elderly receive identical coverage without age-based limits or exclusions.
Are laboratory tests and X-rays free under the Sehat Sahulat Program?
Yes, but only when ordered during a hospital admission. All diagnostic tests, including blood work, X-rays, CT scans, MRIs, and biopsies, receive full coverage if:
- Ordered by the attending doctor after admission
- Performed at the hospital’s laboratory or imaging center
- Medically necessary for your diagnosed condition
Tests ordered at outpatient visits or performed at independent laboratories without hospital admission are not covered.
How do I apply for the CM Punjab free insulin scheme?
No separate application exists for insulin coverage. Diabetic patients automatically qualify for free insulin when:
- Admitted to an empaneled hospital for diabetes-related complications
- Requiring insulin as part of inpatient diabetes management
- Prescribed insulin by the hospital’s attending physician
For outpatient insulin needs, the government’s new doorstep insulin delivery program for Type 1 diabetic patients operates separately. Contact your local health department for information on that initiative.
Does the CM Sehat Program cover dental treatments?
Generally, no. Most dental procedures are explicitly excluded from coverage. The only exceptions involve:
- Dental surgery required due to facial trauma or accidents
- Dental procedures performed as part of hospital admission for related conditions
- Jaw surgery with clear medical necessity
Routine dental care, fillings, extractions, root canals, dentures, and cosmetic dentistry are not covered under any circumstances.

Add a Comment